The post explains the neuroscience of trauma storage to help therapists understand why clients cannot always verbalize their history. The intent is to move beyond “talk therapy” into somatic and nervous system integration.
Q: How is trauma stored in the brain and body?
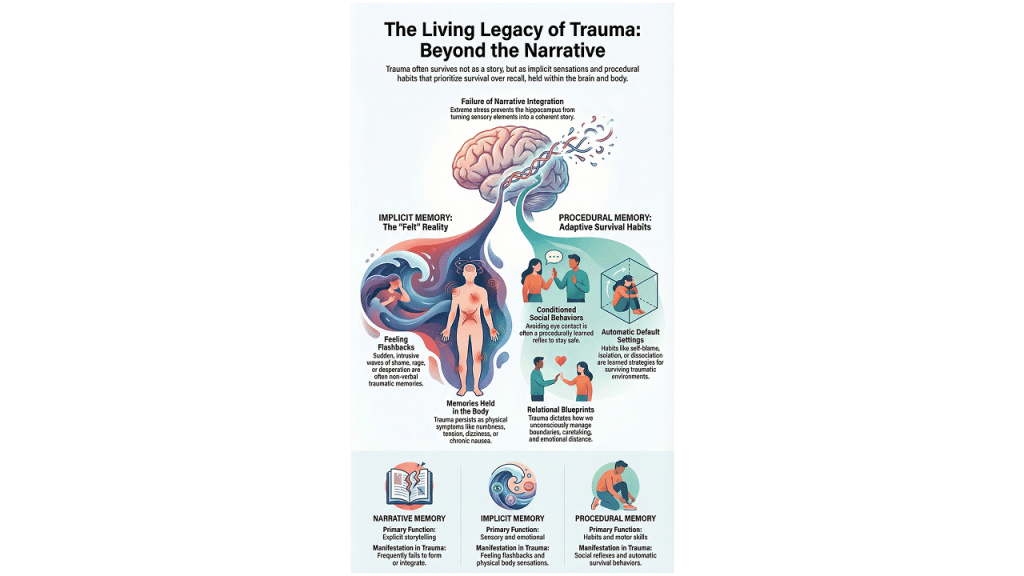
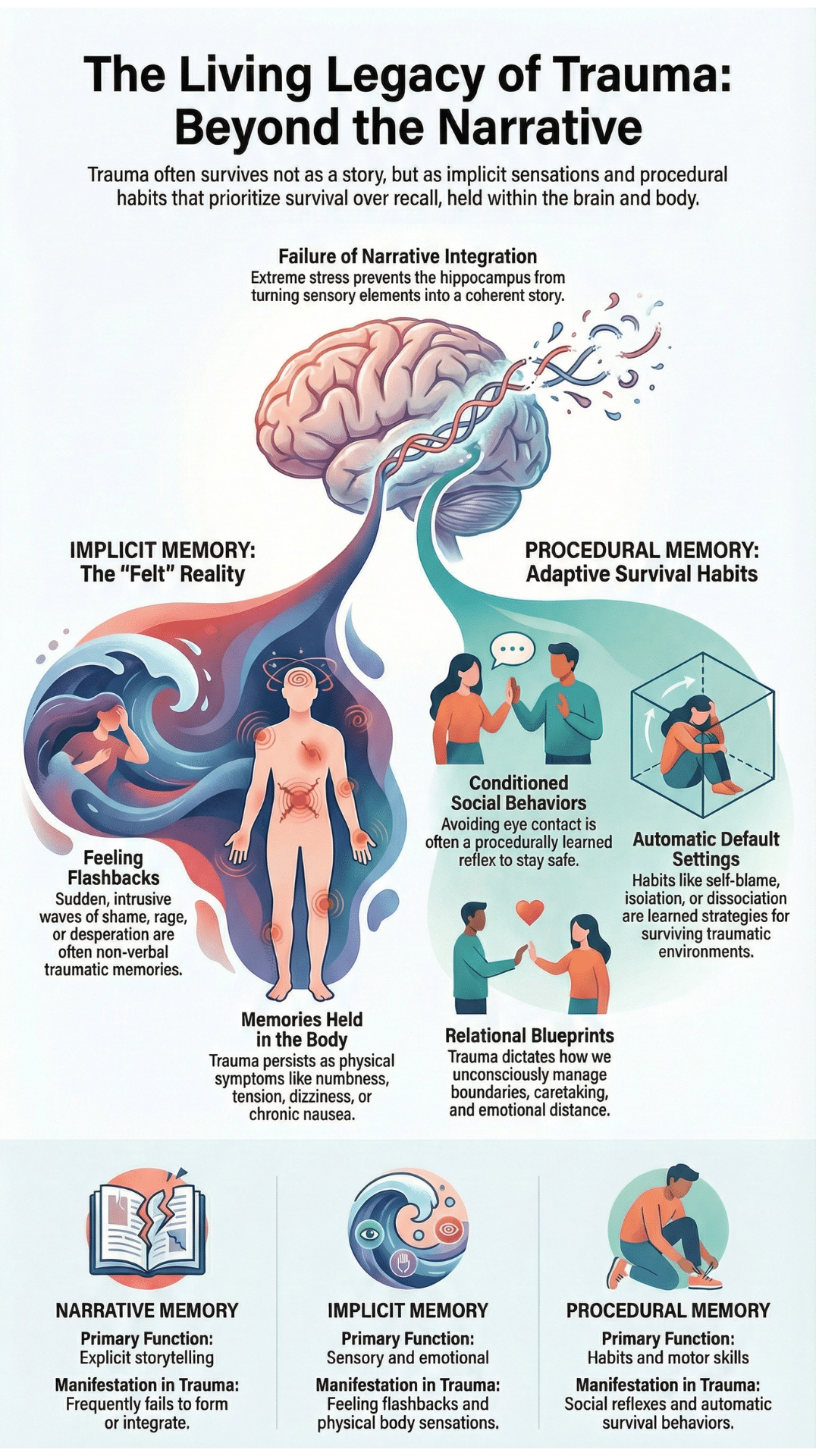
A: Trauma is often encoded as implicit and procedural memory rather than a cohesive narrative. When the hippocampus is overwhelmed by stress, the experience remains fragmented. Healing requires moving beyond insight to address sensory imprints, somatic symptoms, and the survival responses stored within the nervous system.
and somatic encoding is essential for effective trauma processing.
When the Story is Missing: The Reality of Trauma Encoding
In our community of therapists, we often meet clients who feel like they are failing at therapy. They arrive in our offices with a heavy sense of “something is wrong,” yet they cannot point to a clear beginning, middle, or end. They feel broken because they lack a story. As clinicians, we know that trauma is rarely stored as a tidy narrative. It is encoded as a raw, visceral experience.
This distinction matters deeply for the clinical work we do every day. When a client struggles to explain their past, it is not a sign of resistance. It is a biological reality of how the brain handles overwhelming stress.
The Science of Fragmented Memory
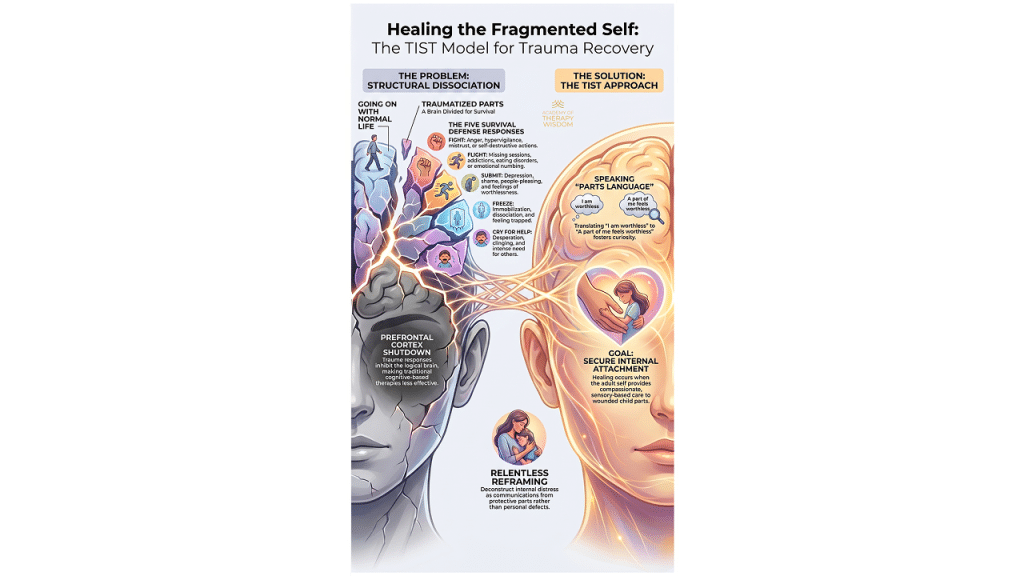
To support our clients, we must look at how the brain processes high-intensity events. Dr. Janina Fisher often points out that healing requires us to look at the fragmented parts of the self. Research from the American Psychological Association confirms that extreme stress disrupts the way we form memories.
The Role of the Overwhelmed Hippocampus
The hippocampus is responsible for time-stamping our lives. It gives us the sense that “this happened back then.” During a traumatic event, this system often goes offline. Instead of a story, the brain captures snapshots. These imprints are sensory and emotional. They are loud, yet they have no words.
Implicit Memory and Felt Reality
Implicit memory is the driver of what we call “felt reality.” This is where flashbacks and somatic waves live. A client might feel a sudden rush of terror in a grocery store without any idea why. Their body is remembering a threat even if their conscious mind has no record of it. This is the intelligence of the somatic therapy lens in action.
Procedural Memory and Survival Strategies
Trauma also lives in our procedural memory. This is the system that handles “how-to” knowledge, like riding a bike or tying a shoe. In a traumatic context, procedural memory encodes survival strategies.
Avoidance, dissociation, and relational pulling are not just “behaviors.” They are automatic defaults. These patterns ensured safety once upon a time. They become relational blueprints that shape how our clients interact with us in the room. When we see a client shut down, we are witnessing a procedural memory of safety.
Moving Beyond Insight in Clinical Work
If trauma is encoded as experience, then insight alone is rarely enough for deep healing. We cannot simply talk someone out of a procedural survival response. We must work directly with the nervous system.
This involves supporting the integration of these fragmented imprints. We help the client move from “I am in danger” to “My body is remembering a time I was in danger.” This shift requires a polyvagal understanding of the state-dependent nature of memory. By honoring the adaptive intelligence of these responses, we create a path toward true reconsolidation.
Healing is about helping the brain and body realize that the event is over. We bridge the gap between the sensory fragment and the present moment. This is the heart of integrative trauma treatment.
Frequently Asked Questions
Why do clients experience flashbacks without memories? This happens because trauma is often stored in the implicit memory system while narrative systems are offline. The body experiences the emotion or sensation of the event as if it is happening now. Working with dissociation helps clients separate these past sensations from their current reality.
Can “talk therapy” alone resolve procedural trauma? Insight can be helpful for understanding patterns, but procedural memory is non-verbal. To change automatic survival responses, we often need to include somatic or experiential techniques. This supports the brain in creating new relational defaults and moving toward neuroplasticity in the nervous system.
How does the nervous system drive interpersonal expectations? The nervous system uses past experiences to predict future safety. If a client’s procedural memory associates closeness with danger, they will automatically trigger a defense response in session. Recognizing this as an adaptive strategy allows us to work with the client’s neuroception to build a felt sense of safety.

Join Dr. Janina Fisher for a FREE webinar
Healing the Fragmented Selves of Trauma Survivors
In this free webinar, Dr. Janina Fisher will help you:
How to identify and work with fragmented selves in trauma survivors.
How to stabilize chronically at-risk clients using TIST principles.
How to address self-alienation and dissociation to foster self-acceptance.
How to navigate therapeutic gridlock and work effectively with resistant, stuck, or emotionally overwhelmed clients.