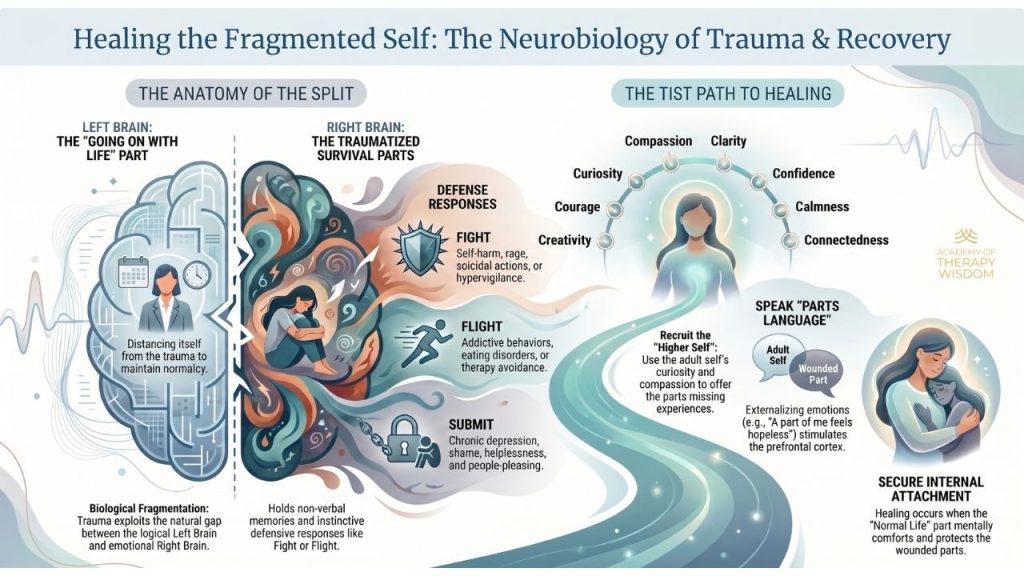
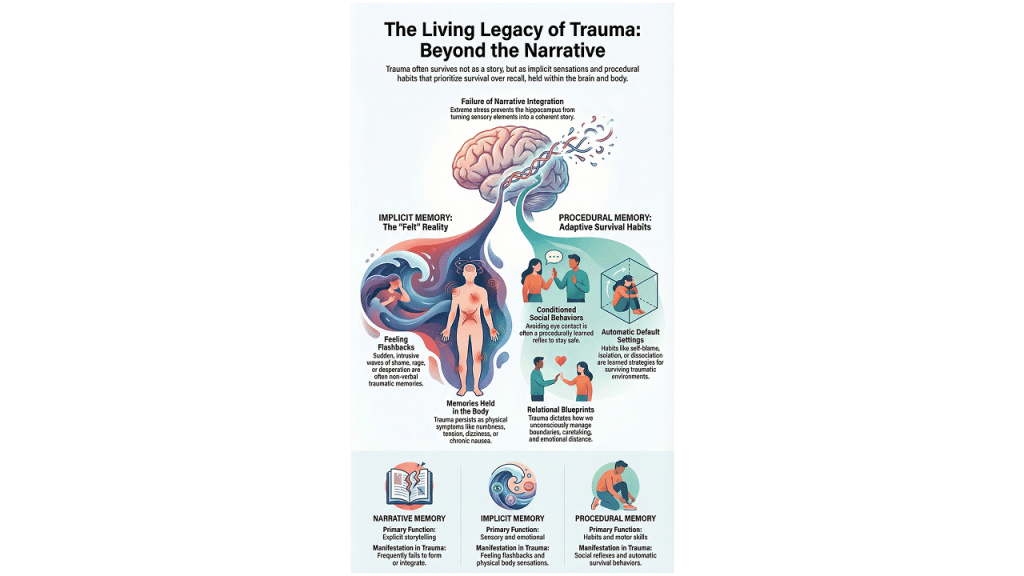
An excerpt from the therapist online training course Trauma Informed Stabilization Treatment (TIST) Introductory Webinar led by Dr. Janina Fisher, Ph.D.
Trauma therapists frequently encounter clients whose treatment is complicated by their addictive behavior, self-harm, or suicidality. The meaning they have made of these patterns is
“My life is not worth living” or “I do this to punish myself” or “It’s the only way I get relief.” The result of these conclusions is to fuel the impulses to do it again and again. In order to help these clients, we have to help them find a different way of understanding their self-destructive impulses.
Trauma-related symptoms always reflect adaptations that helped our clients to survive.
We always have to look at symptoms as having had a purpose and we have to admire the symptom as a survival resource. With symptoms related to trauma, there is always meaning. Hopelessness might be a feeling memory of a child trapped in a dangerous world without comfort, safer in feeling hopeless than in feeling hope only to be disappointed again and again. Shame might be a feeling memory of feeling humiliated by the abuse or a feeling that facilitates compliance and increases safety a little bit more. The wish to die might be a valiant attempt to exert some sense of control.
When I ask clients,
“How did the shame help you survive?”
They almost always say, “I don’t know what you mean. How could it have helped me survive?” And I say,
“Well, when you feel ashamed, what happens?” And they say,
“I feel this kind of this huge flushing of heat. I get beet red. And then I just want to sink through the floor. I can’t speak.” And I say,
“Okay, how did that help you survive?” And then they think,
“Oh yes, it was safer to be unable to speak. It was safer to want to shrink into a hole. It was safer to be seen and not heard.” And then they get it: “Oh, so the shame took away my voice and that was safer.”
Then I can say: “So really you owe that ashamed part a debt of gratitude. Without it, you might have said too much. You might have been too visible.”
Self-harm Had Value for Trauma Survivors
We have to think about that in terms of parts. There’s no value in today’s world in my client becoming voiceless, turning away, not being able to meet the gaze of others. There’s no value now, but there was then. There’s no value now in my client’s suicidal fantasies, but there was value then.
Suicidal symptoms represent what I call an exit plan or a parachute. Wanting to die was often the one remaining hope that our clients had: the one thing that could give them a way out, a way of controlling what was happening. So I can say,
“Yes the suicidal part is offering to help you out. It’s offering you a parachute. It may not trust that you can handle the intense emotions and memories.”

Join Trauma Informed Stabilization Treatment Webinar by Dr. Janina Fisher
Helping Trauma Survivors Get Unstuck: A Fragmented Selves Approach in Therapy
In This NEW Janina Fisher Webinar you will learn:
How to understand perplexing clients using the TIST perspective so you can see the fragmented selves at work.
How to organize a treatment plan using the TIST model so you have an effective approach to care.
How TIST helps shift even the most stuck clients so they can finally make progress.
How to relieve your frustration and prevent burnout with more effective trauma treatment.
on April 4, 9-10am PDT / noon-1pm EDT / 5-6pm BST
The Biology of Trauma Survivors’ Symptoms
Any type of self-injury—headbanging, cutting, burning, swallowing, the whole array—works because when we cause pain to the body, it triggers an adrenaline response which creates a sense of being calm, cool, collected, somewhat distant from what we’re experiencing. Adrenaline also increases feelings of energy and power in the body. With any type of injury, we also produce endorphins. Endorphins are the happy neurochemicals in the body, creating. a sense of relaxation. The pain is gone, and we feel good. No wonder self-injury has been an issue for probably hundreds of years.
We can also reframe depression. When I ask clients,
“How did the depression help you survive?” Most of them say,
“Oh, it was like my cave. I could hide inside it. It was like a cocoon. It buffered me from what
was happening.”
The traditional ways of helping people who struggle with suicidality, self-injury, eating disorders and addiction is to say, “You are harming yourself. You are threatening your life.” That has never worked terribly well. It certainly is the basis for most treatment programs, but it hasn’t been as effective as we would like.
Addressing self-destructive patterns as ingenious survival responses changes the client’s relationship to them. Traumatized clients may not care if they live or die, but they do respond to reminders that it took courage and creativity to survive.
To learn more about how Janina Fisher developed her revolutionary model for treating self-harm, eating disorders, addiction, suicidality, and other self-destructive behaviors by working in state hospitals with clients who weren’t seeing results from other therapies, see The History of Healing the Fragmented Selves with TIST. To learn about certification in this model, go to Trauma Informed Stabilization Treatment (TIST) Introductory Webinar