Exploring the neurobiological shift from narrative memory to somatic storage in trauma survivors.
Q: How does trauma become a living legacy in the body?
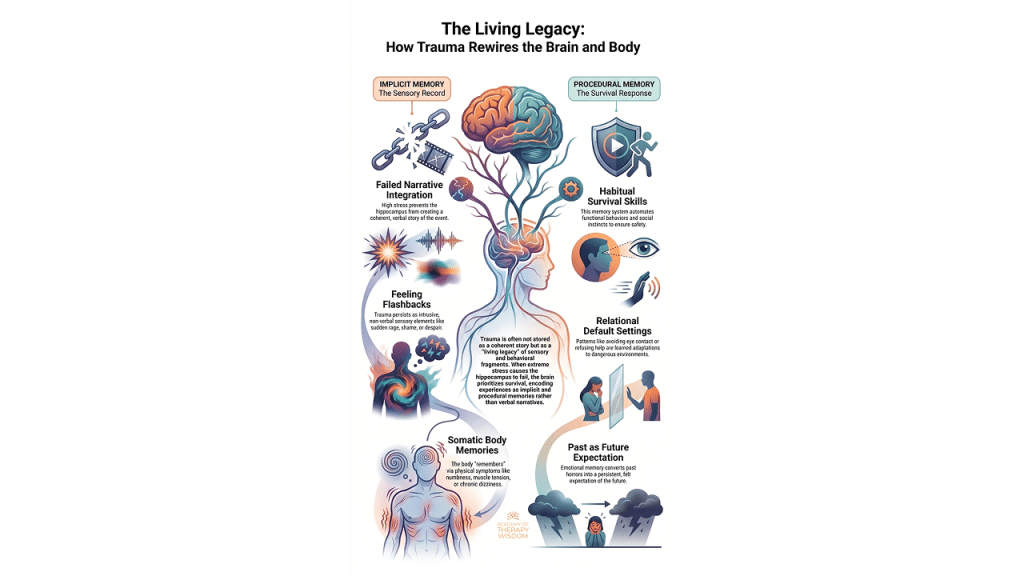
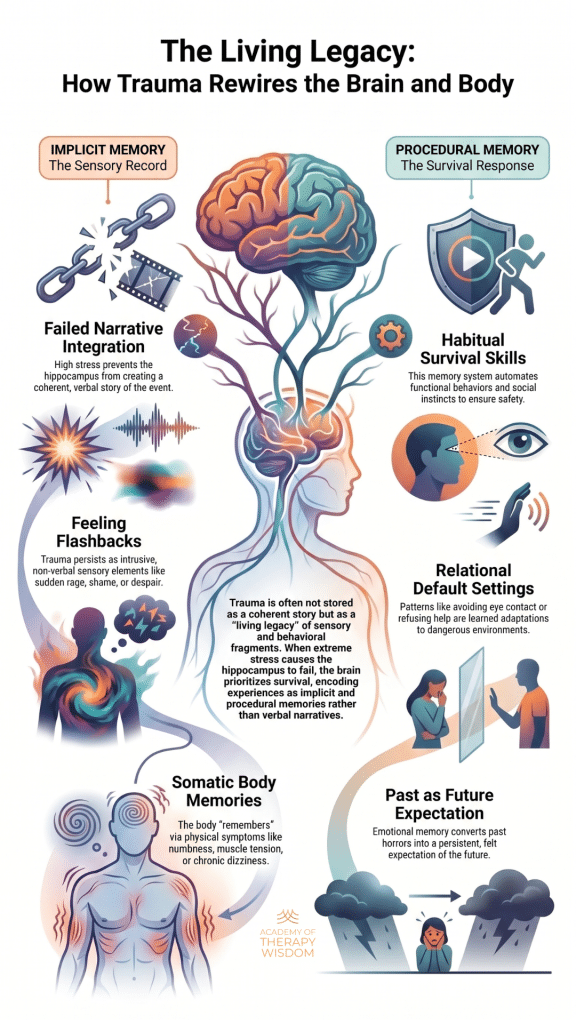
A: Trauma becomes a living legacy when high stress overwhelms the hippocampus, preventing the formation of a clear story. Instead, the brain encodes the experience as implicit sensations and procedural survival habits, such as hypervigilance or muscle tension, which persist long after the threat has ended.
as sensations and survival responses within the body.
Moving Beyond the Narrative Story
In our community of therapists, we often see clients who feel stuck because they cannot “talk” their way out of their pain. We know that trauma isn’t always remembered as a story. It often shows up as a collection of sensations and automatic responses that stay in the nervous system. This happens because the brain has a specific way of prioritizing survival over storytelling when things get overwhelming.
When a person faces a traumatic event, the hippocampus may go offline. This part of the brain is responsible for giving our lives a sense of time and place. Without it, the brain cannot build a coherent narrative. Instead, the experience is pushed into other systems. We call this the living legacy of trauma. It means the past stays present because the body hasn’t been told that the danger is over.
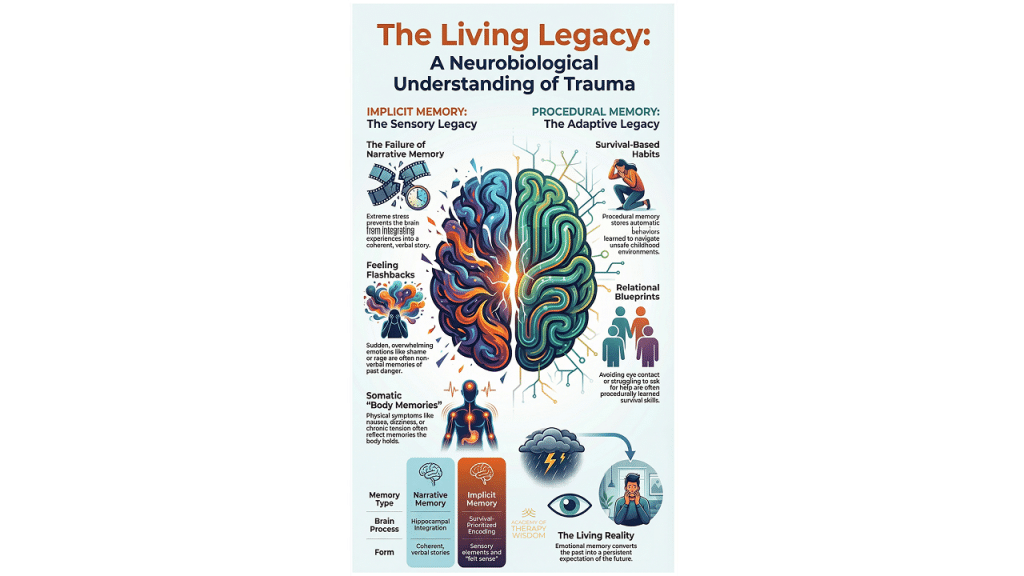
Implicit Memory and the Sensory Record
One of the most common ways this “living legacy” appears is through implicit memory. This is the sensory record of the event. It does not come with words or a clear beginning and end. Instead, it surfaces as emotional flashbacks. A client might suddenly feel a wave of deep shame or a spike of rage that seems to come out of nowhere.
These feelings are actually fragments of the past. Because they are stored as implicit memory, they feel like they are happening right now. As clinicians, we must help clients recognize these waves as memories held by the body rather than a reflection of their current reality. This shift in perspective is a huge part of trauma-informed stabilization treatment developed by experts like Dr. Janina Fisher.
Procedural Memory and Survival Habits
While implicit memory holds the feelings, procedural memory holds the actions. These are the survival-based habits that the brain develops to stay safe. You might notice these in your office as a client who constantly scans the room or someone who finds it impossible to maintain eye contact.
These aren’t just personality traits or “difficult” behaviors. They are automatic patterns. The nervous system has learned that withdrawal or hypervigilance is the best way to survive. Over time, these patterns become relational default settings. They shape how our clients see connection and safety. To help a client change these habits, we have to work with the polyvagal state of the nervous system rather than just the thoughts in their head.
The Body as the Keeper of Memory
The body often reflects what the mind cannot speak. Somatic symptoms like chronic muscle tension, dizziness, or a constant feeling of numbness are often the body’s way of holding an unintegrated memory. These defensive postures are the physical manifestation of c-ptsd and structural dissociation.
To support true integration, we need to move toward experiential work. By focusing on the “how” of the body rather than the “why” of the story, we can help clients move toward neuroplasticity and healing. We are looking for a way to help the fragmented parts of the self find a sense of safety and self-energy again. This is the heart of the work we explore here at the Academy of Therapy Wisdom.
Frequently Asked Questions
How does hippocampal impairment affect trauma recovery? When the hippocampus is overwhelmed, it cannot timestamp memories correctly. This leads to trauma feeling “ever-present” in the body. Recovery involves using somatic therapy to help the nervous system understand that the event is in the past.
What is the difference between implicit and procedural memory in therapy? Implicit memory is the sensory and emotional “feeling” of the trauma. Procedural memory is the “action” or habit used to survive it. Both require moving beyond cognitive talk therapy to reach the deeper systems of the brain.
How can therapists work with the “living legacy” of trauma? Therapists can use parts-work and somatic interventions to identify sensory fragments. By focusing on neuroception and safety, we help clients integrate these memories into a narrative that no longer feels threatening to their current life.
What you´ll learn:
- Vestibular Engagement for Emotional Regulation
- Using the Eyes to Hack the Stress Response System
- Subtle Sounds to Release the Peri-Trauma Response
- Effective Self-Holding and Self-Swaddling Techniques
- How and When to Apply Bilateral Stimulation
- Integration and Completing the Stress Response Cycle