The intent of this post is to provide therapists with a deep understanding of non-verbal memory systems. By distinguishing between implicit sensory fragments and procedural survival habits, clinicians can better support clients whose trauma is stored in the body rather than in a clear narrative.
Q: How does trauma affect implicit and procedural memory?
A: Trauma disrupts narrative integration, causing experiences to be stored as implicit sensory fragments (emotions/sensations) and procedural habits (automatic survival behaviors). Healing requires working with the nervous system to address these “feeling memories” and “relational blueprints” that exist beyond cognitive insight.
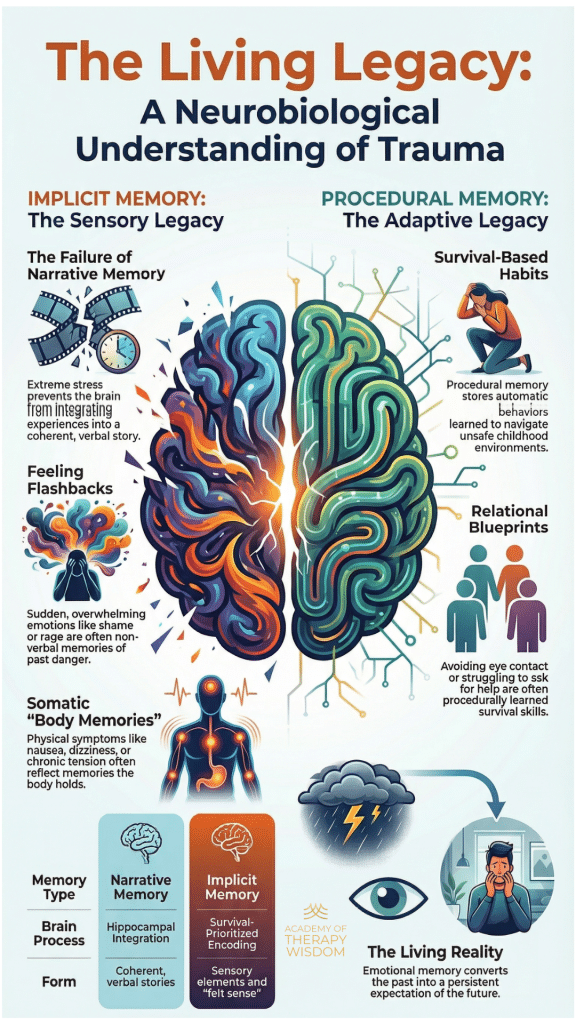
sensory fragments and survival-based habits.
The Living Legacy of Unintegrated Experience
In our community of therapists, we often see clients who struggle to put their pain into words. They might describe a sudden wave of shame or a physical tightening in the chest that seems to come from nowhere. This happens because trauma doesn’t just live in the stories we tell. It shapes the very way the brain and body learn to stay alive.
When a person faces overwhelming stress, the brain sometimes fails to build a clear, chronological story of the event. Instead of a memory that has a beginning, middle, and end, the experience is broken into pieces. These pieces are held in two specific systems: implicit and procedural memory.
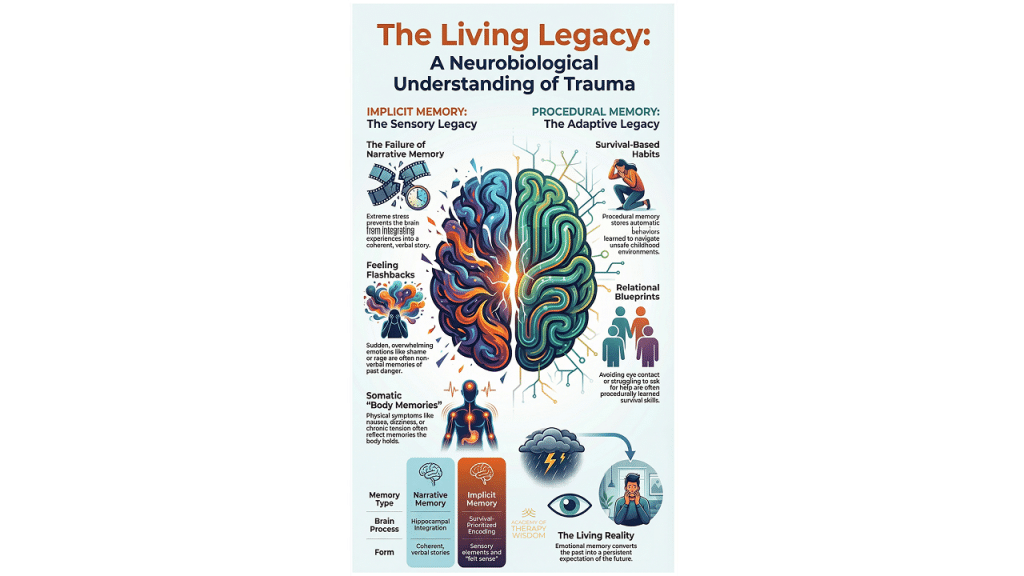
Implicit Memory: The Sensory Legacy
Implicit memory is where our “feeling memories” reside. These are non-verbal and sensory-based. For a survivor, an implicit memory might feel like a sudden flash of rage or a deep sense of fear that doesn’t have a label.
Because these fragments are stored in the nervous system, they often feel like they are happening in the present moment. A client isn’t just remembering a past event; their body is re-experiencing the sensory legacy of that event. This can lead to dissociation or emotional flashbacks that feel entirely disconnected from their current surroundings.
Procedural Memory: The Adaptive Legacy
While implicit memory holds the feelings, procedural memory holds the actions. The brain is brilliant at learning how to survive. It develops automatic behaviors to navigate danger. This is what we call the adaptive legacy.
These behaviors might look like hypervigilance, a constant need to please others, or an automatic tendency to pull away when someone gets too close. Over time, these survival steps become “relational blueprints.” They are the automatic expectations a client has about safety and connection. When we work with somatic therapy, we are often helping the client notice these physical urges before they turn into automatic actions.
Why Cognitive Insight is Not Enough
Understanding why we feel a certain way is helpful, but it rarely changes the body’s stored response. According to Dr. Janina Fisher, a leading authority on Trauma-Informed Stabilization Treatment, healing must involve the nervous system.
If the body keeps the record through tension, nausea, or defensive postures, our work must address that embodied awareness. We have to help clients expand their window of tolerance so they can observe these memory systems without becoming overwhelmed by them. This shifts the focus from “what happened” to “how is your body trying to protect you right now.”
Frequently Asked Questions
How do relational blueprints affect current relationships? Relational blueprints are automatic expectations of danger or rejection based on attachment trauma. They cause the procedural memory system to trigger defensive habits even in safe environments.
Can implicit memories be turned into narrative memories? While we can’t always create a perfect story, we can use memory reconsolidation to take the “charge” out of sensory fragments. This helps the brain recognize the memory as a past event rather than a present threat.
What is the first step in working with procedural trauma responses? The first step is helping the client develop neuroception, which is the ability to sense safety or danger within their own body. This allows them to notice an automatic habit before it takes over.

Join Dr. Janina Fisher for a FREE webinar
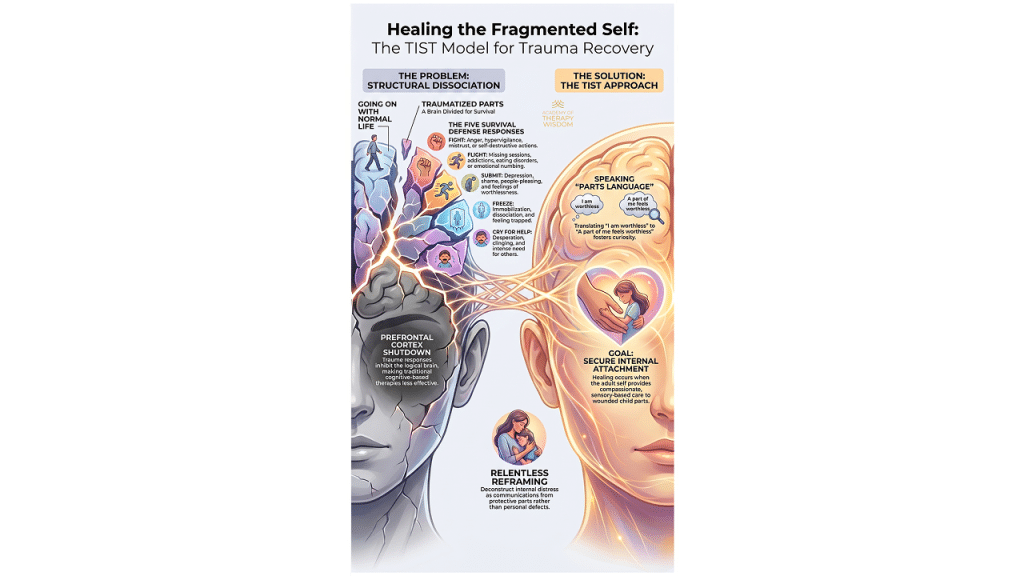
Healing the Fragmented Selves of Trauma Survivors
In this free webinar, Dr. Janina Fisher will help you:
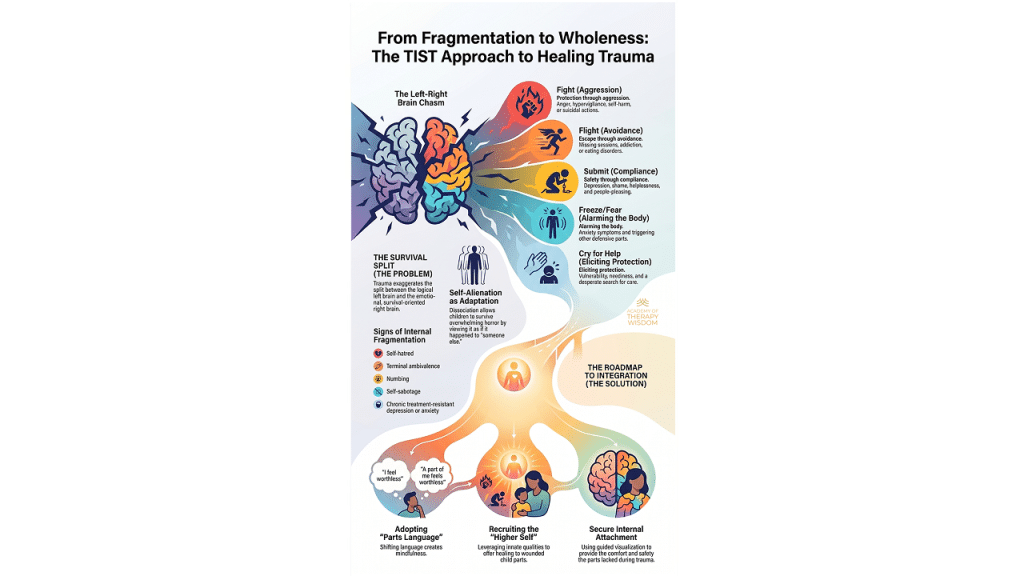
How to identify and work with fragmented selves in trauma survivors.
How to stabilize chronically at-risk clients using TIST principles.
How to address self-alienation and dissociation to foster self-acceptance.
How to navigate therapeutic gridlock and work effectively with resistant, stuck, or emotionally overwhelmed clients.