Why State Leads the Story: A Guide for Trauma Clinicians
Q: What does “state creates story” mean in trauma therapy?
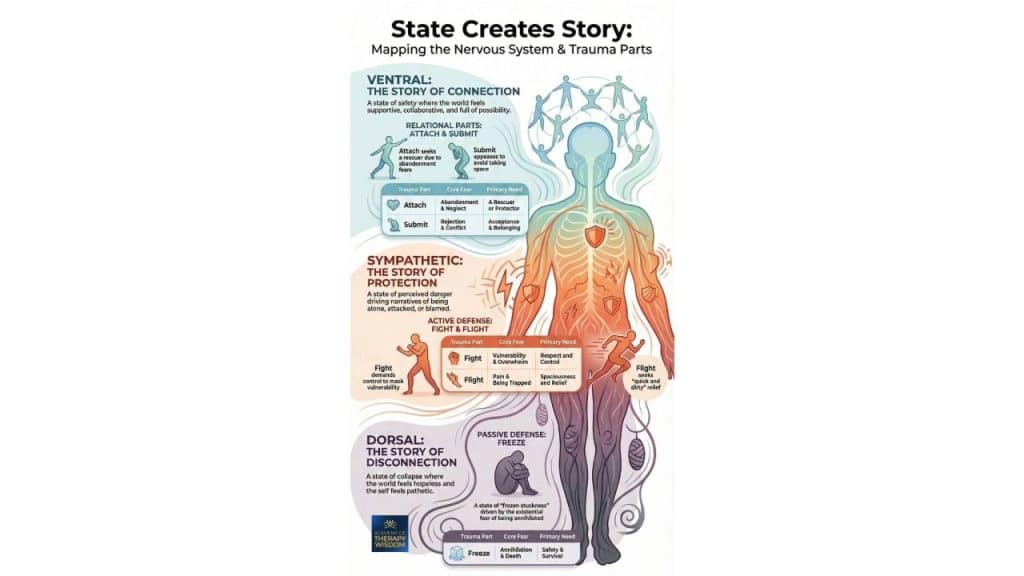
A: In a polyvagal-informed framework, “state creates story” means that a client’s narrative and beliefs are filtered through their current autonomic nervous system state. A sympathetic state generates stories of danger or conflict, while a dorsal state produces stories of hopelessness or “stuckness.”
Tracking the Autonomic Narrative in the Therapy Room
In our community of therapists, we know that what a client says is often less important than the physiological state they say it from. When we partner with experts like Linda Thai, we are reminded that our clients’ stories don’t emerge in a vacuum. Instead, the autonomic nervous system organizes the world before the thinking brain even has a chance to catch up.
When we talk about “state creates story,” we are acknowledging that the body’s quest for safety dictates the mind’s interpretation of reality. For practitioners, this shift in focus is life-changing. It moves us away from trying to “talk a client out” of a belief and toward helping them shift the underlying physiology that makes that belief feel true.
The Three Pillars of the Nervous System Map
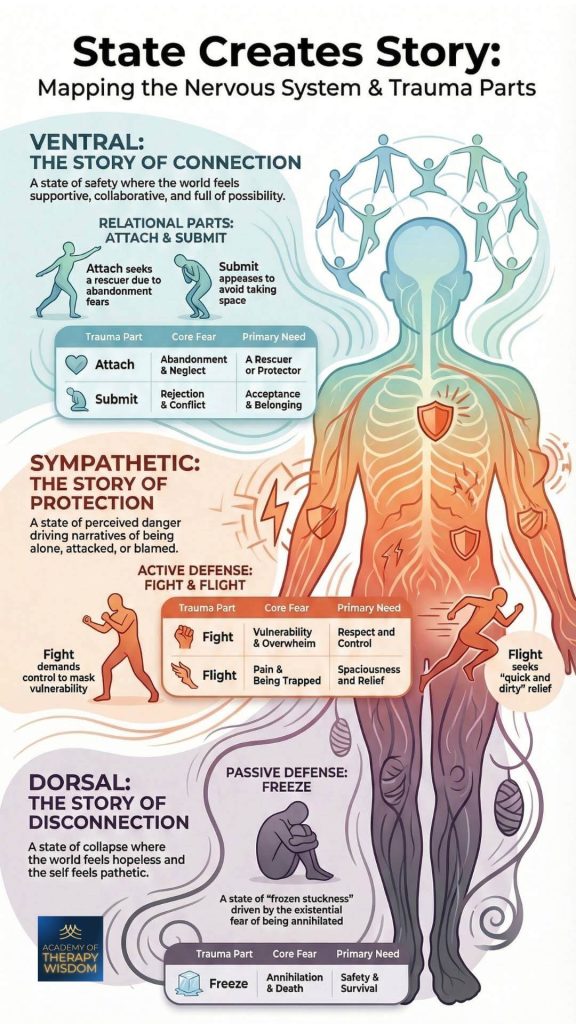
Differentiating between these states allows our interventions to become more targeted and effective. As the infographic shows, each state has its own adaptive logic.
Ventral Connection: The Foundation of Social Engagement
This is the state of safety and connection. In our community, we prioritize helping clients access this “green zone” where curiosity and relational repair become possible. It is the only state where the system feels resourced enough to engage in deep healing work.
Sympathetic Protection: The Energy of Mobilization
When the system detects a threat, it moves into sympathetic activation. This presents as fight or flight. In this state, the client’s story is often one of high emotional tension or a desperate need to “do something.” These behaviors are deeply adaptive responses to perceived danger.
Dorsal Disconnection: The Logic of Collapse
When mobilization fails or the threat is too great, the system may move into a freeze-based collapse. This dorsal state is characterized by numbness, shame, and a sense of being “gone.” Differentiating between attach/submit patterns and true dorsal collapse is a skill we focus on in our advanced trauma training.
Clinical Application: Restoring Ventral Safety
What we hear from practitioners is that healing complex trauma requires a phase-oriented, bottom-up perspective. We cannot ask the brain to change a story if the body is still screaming “danger.”
As Linda Thai emphasizes in her work, our goal is to help clients build the capacity to move flexibly out of protective survival states. This involves fine-tuning our own therapeutic-presence to act as a co-regulatory anchor. When we track these state shifts with precision, we help the client stay within their window-of-tolerance.
Research consistently supports this somatic-informed lens. For instance, studies on polyvagal theory highlight that our neuroception—the subconscious detection of safety—is what ultimately allows for the “un-pairing” of trauma from current experience. By focusing on the body’s signals, we provide a container where the client can move from survival into true social engagement.
Frequently Asked Questions
How can I help a client recognize their state shifts in session? Start by naming the somatic markers you observe. You might say, “I notice your breath getting a bit shallower as we talk about this.” This invites the client to track their internal experience and helps them differentiate between their “story” and their physiological state.
What is the “bottom-up” approach in trauma stabilization? A bottom-up approach prioritizes the body’s sensations and autonomic states before addressing cognitive thoughts. Using tools from somatic-therapy, we help stabilize the nervous system first, which naturally allows the client’s narrative to shift toward safety.
Why is the “attach/submit” pattern often confused with cooperation? In trauma, an “attach/submit” response is a survival strategy where a client complies to avoid conflict. It can look like cooperation but is actually a state of high internal stress. Recognizing this prevents us from pushing a client further into dissociation or overwhelm.
What you´ll learn:
- Vestibular Engagement for Emotional Regulation
- Using the Eyes to Hack the Stress Response System
- Subtle Sounds to Release the Peri-Trauma Response
- Effective Self-Holding and Self-Swaddling Techniques
- How and When to Apply Bilateral Stimulation
- Integration and Completing the Stress Response Cycle