Table of Contents
- Introduction: Why Early Complex PTSD Identification Matters
- Defining and Differentiating Complex PTSD in 2025
- Step 1: Comprehensive Trauma-Focused Assessment
- Step 2: Recognizing the Six ICD-11 Symptom Clusters
- Step 3: Advanced Screening Tools and Neurobiological Markers
- Step 4: Somatic and Cognitive Indicators in Complex PTSD
- Step 5: Cultural and Developmental Considerations
- Step 6: Integrating Findings for Early Intervention
- Conclusion: Building Clinical Excellence in Complex PTSD
Introduction: Why Early Complex PTSD Identification Matters
We´ve learned how challenging and crucial it is to distinguish complex PTSD symptoms early—especially as trauma presentations evolve and new research emerges. Trauma CE requirements are also shifting, with a 2025 emphasis on up-to-date, proven evaluation skills. In this blog, I’ll share actionable, research-driven steps for early recognition, drawing from the latest developments, upcoming best-in-class trainings, and resources to keep your practice at the cutting edge. If you’re ready for advanced PTSD therapy certification, our free online webinar training Healing the Fragmented Selves of Trauma Survivors with Janina Fisher is an excellent place to start.
Defining and Differentiating Complex PTSD in 2025
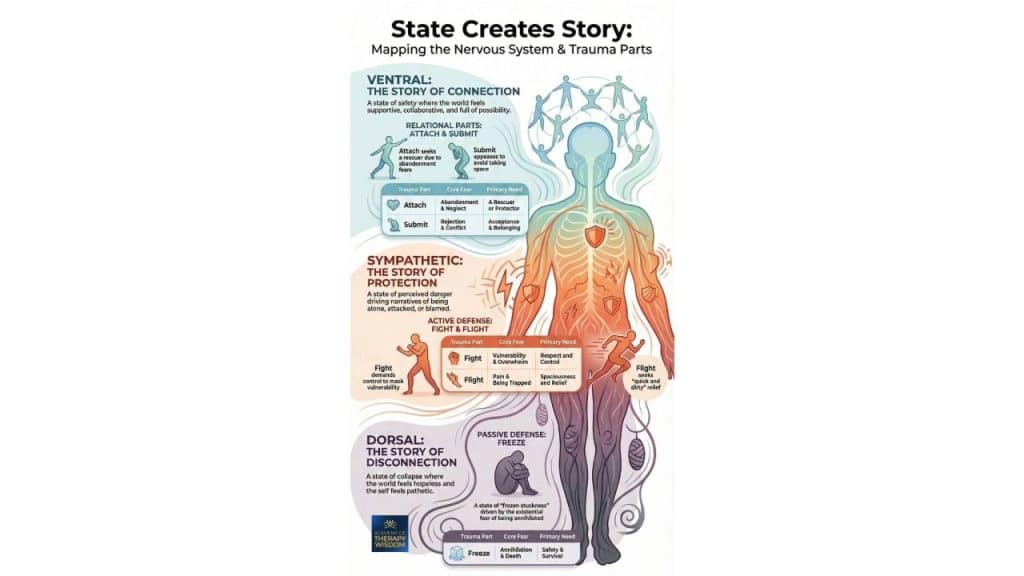
The distinction between classic PTSD and Complex PTSD (C-PTSD) is now codified in ICD-11 and further clarified in DSM-5-TR updates. C-PTSD is characterized by additional symptoms—affect dysregulation, negative self-concept, and relational disturbances—on top of core PTSD criteria (SAGE Journals). Early identification is essential to avoid misdiagnosis and to tailor effective, phase-based interventions.
Step 1: Comprehensive Trauma-Focused Assessment
Start with a full trauma history, including adverse childhood experiences and developmental trauma. The latest Developmental Trauma Disorder 2025 Update highlights the importance of mapping trauma chronologically and contextually (UConn DTD 2025 Update). Key tips:
- Use structured interviews (e.g., Life Events Checklist, ACE-Q) and collateral information.
- Assess for trauma type, chronicity, and attachment disruptions.
- Ask about dissociation, shame, and self-blame—these are often missed but central in C-PTSD.
Step 2: Recognizing the Six ICD-11 Symptom Clusters
Early identification relies on the six ICD-11 symptom clusters for C-PTSD (SAGE Journals):
- Re-experiencing the trauma
- Avoidance of reminders
- Persistent sense of current threat
- Affect dysregulation
- Negative self-concept
- Disturbances in relationships
The new CPTSD-DSO Scale (validated by Beckord et al., 2025) is a brief, reliable tool for distinguishing PTSD, C-PTSD, and overlapping presentations (ScienceDirect).
Step 3: Advanced Screening Tools and Neurobiological Markers
2025 research is illuminating new frontiers in early C-PTSD detection:
- Genomic and Connectome-Based Screening: Recent studies use neurobiological and genomic markers to identify at-risk individuals. The McLean Hospital/NIH project analyzes brain samples for early biomarkers of PTSD/C-PTSD (McLean Hospital).
- Connectome Predictive Modeling: New imaging can detect early neural networks associated with PTSD development (JAMA Network Open).
- Molecular Differentiation: ScienceDaily reports molecular differences in brain processing between direct and witnessed trauma, informing early intervention (ScienceDaily).
Step 4: Somatic and Cognitive Indicators in Complex PTSD
C-PTSD is often somatically encoded. Look for:
- Chronic dysregulation: Hyper- or hypo-arousal, chronic pain, GI issues, or autoimmune symptoms.
- Cognitive symptoms: Dissociation, negative self-appraisal, intrusive thoughts, and impaired memory (Frontiers in Psychiatry).
In Trauma-informed Stabilization Treatment (TIST) and other leading approaches, somatic tracking and body-based assessment are now considered best practice.
Step 5: Cultural and Developmental Considerations
Cultural humility is essential for accurate diagnosis. The latest trauma CE trainings emphasize:
- Developmental Trauma: Early maltreatment, neglect, and attachment disruptions are strong predictors for C-PTSD (UConn DTD 2025 Update).
- Cross-Cultural Tools: Use validated tools in the client’s language and context, and consult with culturally-matched clinicians when needed.
- Cross-cultural instruments should examine locally relevant reactions, such as idioms of distress and explanatory models of illness, and account for ongoing stress and adversity (Patel and Hall, 2021).
Step 6: Integrating Findings for Early Intervention
Once symptoms are identified, phase-based stabilization is critical. TIST’s protocols—grounded in Janina Fisher’s work—prioritize internal safety, psychoeducation, and collaborative treatment planning. For therapists, this means:
- Providing clear, validating feedback on assessment results
- Starting with stabilization and skills training before trauma processing
- Using parts work, somatic interventions, and relational repair
As Janina Fisher notes,
“Integrating the disowned parts of ourselves is the cornerstone of trauma recovery.”
—Healing the Fragmented Selves of Trauma Survivors
Recent Research, Conferences, and New CE Resources (2025)
Fresh Research (2024–2025):
- Developmental Trauma Disorders 2025 Update
- Groundbreaking PTSD Biomarker Study – McLean Hospital (NIH)
- CPTSD-DSO Scale Validation (ScienceDirect, 2025)
New Conferences (2025) for live and replay attendance:
- 1st Annual PTSD Research Conference: May 5–6, 2025, Boston, MA
- Trauma-Informed Care Conference: Feb 19, 2025, Chester Street Foundation
- Innovations in Psychotherapy 2025: Anaheim & Online, October 8–11, 2025
Cutting-Edge CE Trainings & Resources:
- Trauma-informed Stabilization Treatment (TIST) Certification Program (with Trauma CEs)
- Trauma Resiliency Model (TRM) Level 2, Aug 2025
- PTSD: National Center for PTSD – Free Professional CE (1 Hour)
- Trauma Resource Institute CRM Teacher Training, Mar 2025
The exit surveys show an overwhelming support for not only the techniques offered by Janina Fisher in our TIST certification training, which remains a top training program at the forefront for complex trauma work, but they also herald the highly supportive teaching methods and community found there. Naturally, we include this training on any best-of trauma ce list! We´re biased, I know. But results don´t lie, and TIST is our most popular course. Janina Fisher is a treasure, and offers us incredible science-backed, successful outcomes-based methods in trauma treatment.

Join Dr. Janina Fisher for a FREE webinar
Healing the Fragmented Selves of Trauma Survivors
In this free webinar, Dr. Janina Fisher will help you:
How to identify and work with fragmented selves in trauma survivors.
How to stabilize chronically at-risk clients using TIST principles.
How to address self-alienation and dissociation to foster self-acceptance.
How to navigate therapeutic gridlock and work effectively with resistant, stuck, or emotionally overwhelmed clients.
Conclusion: Building Clinical Excellence in Complex PTSD
As I reflect on the latest research and evolving best practices, it’s clear that early identification of complex PTSD is both an art and a science—one that demands ongoing learning and humility. By integrating advanced assessment, leveraging new neurobiological insights, and using phase-based interventions, you can transform outcomes for your most vulnerable clients. If you’re ready to master these skills and join a vibrant community of trauma therapists, while also earning required trauma ceus, Janina Fisher´s free introductory training Healing the Fragmented Selves of Trauma Survivors is an ideal next step.
Here’s to your continued growth as a trauma specialist in 2025 and beyond! On behalf of the entire Therapy Wisdom team dedicated to your growth and wellbeing as a therapist and person, thank you for dedicating yourself to helping others heal. We look forward to welcoming you into our community and supporting you in every way that we can.
Cheers!
Heather